I still remember the first visit with a patient I will call Laura. Mid 40s, a demanding job, two kids, and a calendar that looked like a game of Tetris. She had tried every reasonable diet, filled a closet with fitness gadgets, and wore an expression I would describe as politely resigned. Her labs told a story her willpower could not change on its own: fasting insulin elevated, triglycerides drifting up, A1c at 5.9%, and a waist circumference that had expanded despite taking more steps than most people I know. That first day, she exhaled and said, I swear my body is working against me. She was right. And it is exactly what an insulin resistance weight loss program is built to reverse.
This is not a generic diet or a pep talk. When weight gain is tangled with insulin signaling, hormones, sleep, stress, and sometimes genetics, you need a structured, medically supervised weight loss program that puts biology first and motivation second. The order matters.
What insulin resistance really means for your body
Insulin’s job is to move glucose into cells and keep blood sugar in a safe range. With insulin resistance, your muscle, liver, and fat cells respond weakly to insulin’s message. The pancreas compensates by making more insulin. Elevated insulin is not just a number on a lab report. It changes how your body handles energy: it shifts fuel toward storage, makes fat breakdown harder, drives hunger in some people, and blunts satiety signals in others. Over time, the liver makes more triglycerides, and the brain’s appetite centers can become less responsive to subtle stop-eating cues.
You can be insulin resistant with normal fasting glucose. Early warning signs show up as elevated fasting insulin, increasing waist size, post-meal fatigue, stubborn plateauing weight, skin tags, acanthosis nigricans at the neck or underarms, irregular cycles with PCOS, or a creeping A1c in the “pre-diabetes” zone. It is not a character flaw. It is physiology.
Why the scale will not budge until insulin does
I meet a lot of determined people who report white-knuckle calorie restriction and longer workouts, then they gain it back at alarming speed. When insulin runs high, your body does everything it can to defend fat mass. Two things often happen. First, hunger signals increase and protein leverage gets ignored when meals are too carb heavy and low in protein, so you are never quite full. Second, the ability to access stored fat for fuel is impaired, so energy dips feel worse and you reach for snacks. If you eat less but your hormonal drivers are misaligned, your resting energy expenditure can fall by 5 to 15 percent within weeks. That is how a calorie deficit fails in practice, even if it looks sensible on paper.
A targeted, physician supervised weight loss plan addresses these drivers head on: insulin, appetite hormones, sleep, stress, and inflammation. Strategy, not willpower, makes the difference.
The nuts and bolts of a clinically supervised weight loss program
A good medical weight loss clinic does not hand out a shake mix and hope for the best. The first visit should feel like an evaluation, not a sale. Expect a detailed history, medication review, body composition assessment, and lab work. I tell my patients that we will write the plan only after we see the map.
https://www.google.com/maps/d/u/0/edit?mid=17dJJj-ZpxDb3nZiHyyBAqsetPdMm0GE&ll=40.8110028643038%2C-74.65744999999998&z=13For insulin resistance, the most useful starting labs include fasting glucose and insulin, A1c, lipid panel with triglycerides and HDL, liver enzymes, TSH and free T4, vitamin D, and sometimes fasting C-peptide. In select cases, we add an oral glucose tolerance test with insulin measurements to quantify the response, particularly when symptoms are strong but fasting numbers are borderline. If PCOS is suspected, we check androgens. If sleep apnea is likely, we arrange a sleep study. Every one of these data points can change the treatment plan.
In a comprehensive weight management clinic, the treatment layers are chosen to support each other. Food choices lower insulin exposure, activity increases insulin sensitivity, sleep and stress work quiet the hormonal noise, and, when appropriate, medications rewire appetite and improve glycemic control. The program is doctor guided, but ownership rests with the patient. You live the plan.
Nutrition that lowers insulin without wrecking your day
There is no single prescription that fits Chester NJ medical weight loss every person with insulin resistance, but there are consistent themes that work in clinic after clinic.
Start with protein. Most adults do better at 1.2 to 1.6 grams per kilogram of ideal body weight per day. In real terms, that is often 90 to 130 grams daily, split across three meals. A protein forward breakfast matters more than people think. A plate with 30 to 40 grams of protein stabilizes glucose and decreases mid-morning cravings. Try Greek yogurt with chia and berries, egg and veggie scramble with a side of cottage cheese, or a whey or pea protein smoothie plus a handful of walnuts.
Shape carbohydrates to your insulin response. Rather than tallying every gram, I use ranges. For many insulin resistant adults, 20 to 40 grams of slow carbs per meal works well, with the lower end on rest days and the higher end on heavy activity days. Choose minimally processed carbohydrates that come with fiber: beans, lentils, steel-cut oats, intact whole grains, fruit, and starchy vegetables in measured amounts. Aiming for 25 to 35 grams of fiber daily improves glycemic control and satiety. When people think low carb and end up low fiber, they feel awful and quit.
Do not fear fat, but be precise. Olive oil, avocado, nuts, seeds, and fatty fish land well, especially when paired with protein and vegetables. The goal is not to drown salads in dressing. It is to provide enough fat to carry flavor and blunt glucose spikes.
Meal timing can help, but it is not magic. A 12 to 14 hour overnight fast paired with an early dinner supports insulin sensitivity for many people. Longer fasts can backfire in those with high stress, disrupted sleep, or a history of disordered eating. If you lift or do high intensity intervals, put more of your carbs near the workout and a larger protein serving afterward.
What a day might look like for an office worker with an evening walk: breakfast of 2 eggs, 1 cup egg whites with spinach and peppers, a side of Greek yogurt topped with 1 tablespoon chia and 1 cup blueberries. Lunch of a large salad with mixed greens, grilled chicken thigh, a half cup chickpeas, sunflower seeds, olive oil and lemon, and a slice of whole grain bread. Dinner of salmon, roasted broccoli, a small sweet potato, and a mixed green side salad. Late snack, if needed, is cottage cheese with cinnamon. Water, black coffee or green tea, sparkling water with a splash of citrus. Alcohol is best kept to weekends at one drink or less. Spirits without sugary mixers cause fewer glucose excursions than beer or sweet wine.
Exercise that trains insulin sensitivity
You will not out-exercise a high insulin state, but training turns the dial. Three types of movement work in concert. First, resistance training two to three days per week to build and protect lean mass. Focus on compound lifts you can progress safely: squats or leg press, hinge pattern like deadlifts or hip thrusts, rows and presses, and loaded carries. If you are new, machines are fine and often safer.
Second, frequent low intensity movement, what we call zone 2 cardio: a brisk walk where you can talk but not sing, light cycling, or swimming, 150 to 300 minutes weekly. Third, a brief dose of higher intensity intervals once or twice per week, especially after a medical clearance if needed. Intervals increase GLUT4 translocation in muscle and improve insulin sensitivity out of proportion to their time commitment. Start small: four rounds of 30 seconds hard, 2 minutes easy.
One overlooked trick is a 10 to 15 minute walk after meals. Post-meal movement tamps down glucose and insulin spikes and often pays better dividends than an extra 30 minutes at the gym done at the wrong time of day.
Medications and medical weight loss injections: when and how they fit
Nutrition and activity lay the foundation. For many patients with insulin resistance, especially with prediabetes, PCOS, or a significant weight history, medication makes the plan sustainable. The public conversation often jumps straight to weight loss injections. They are important, but they are not the only option.
Metformin remains a workhorse. It reduces hepatic glucose production and improves insulin sensitivity. In clinic, we start low and go slow to limit GI side effects. Typical dosing can reach 1,500 to 2,000 mg daily if tolerated. The expected weight change is modest by itself, often 2 to 3% of body weight over several months, but it smooths appetite and reduces cravings for some patients and supports other interventions.
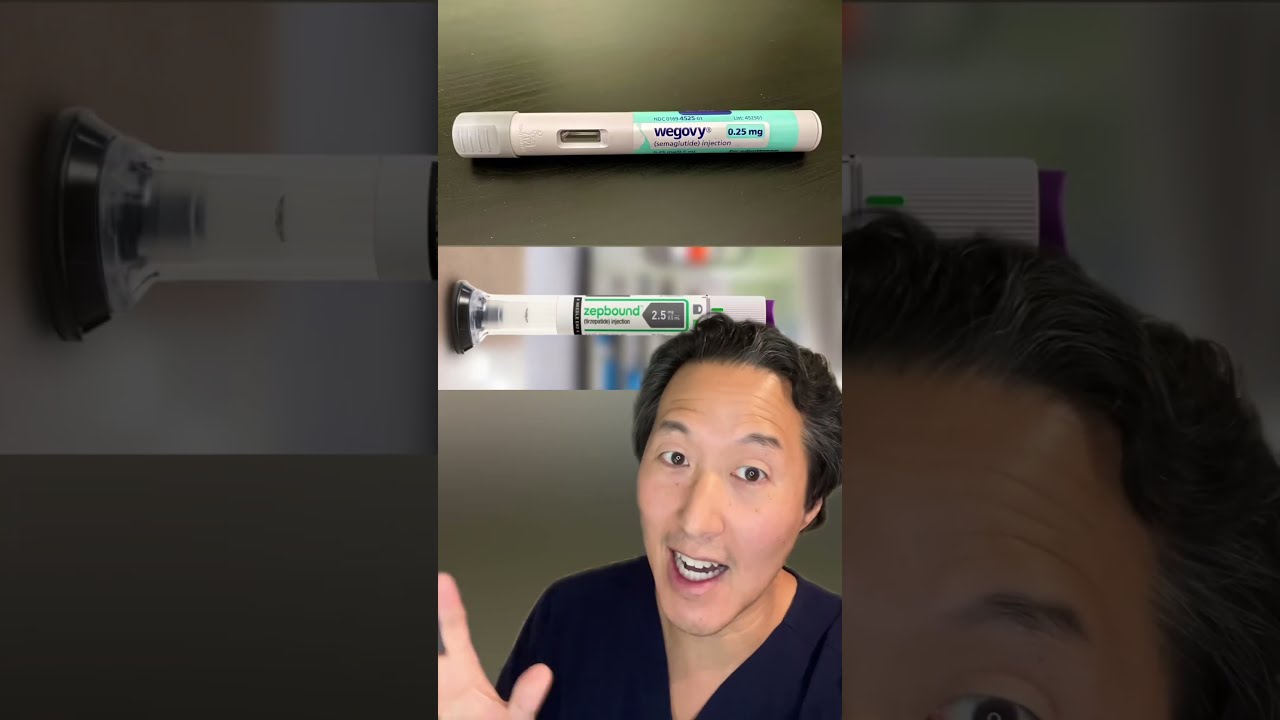
GLP 1 based therapies are now core tools for a prescription weight loss program, particularly for patients with elevated cardiovascular risk or A1c trending up. Semaglutide in an obesity dose is titrated weekly from 0.25 mg to a maintenance dose that can reach 2.4 mg. Tirzepatide, a dual GIP and GLP 1 agonist, starts at 2.5 mg weekly, with maintenance often at 10 to 15 mg. In trials, average weight reductions range from 10 to more than 20% at one year depending on dose and adherence, with improved A1c and triglycerides. In real practice, I see a range. Patients who pair medication with a structured medical diet program and resistance training keep more lean mass and reach higher percentages.
Side effects are real but often manageable: nausea, early fullness, reflux, constipation or diarrhea. We spend time on meal pacing, smaller portion sizes, hydration, and fiber. Rare but serious issues like pancreatitis and gallbladder disease require careful screening. A personal or family history of medullary thyroid carcinoma or MEN2 is a contraindication. Good clinics discuss these points upfront.
SGLT2 inhibitors, approved for diabetes, can modestly support weight loss and cardiometabolic risk in select patients, but they are not first line for weight loss alone and need education about genital infections and hydration. For some patients with binge eating patterns, certain medications that modulate reward circuitry can help. Decisions are individualized by a weight loss doctor who sees the full picture.
I am often asked about rapid medical weight loss. Quick results have motivational value, but speed trades off with lean mass. We can accelerate early losses in a safe fat loss program doctor setting when the patient is high risk ahead of surgery or needs to jump start adherence, usually with a higher protein, lower calorie plan overseen by a physician supervised weight loss team, with electrolytes and bloodwork monitored. Most patients do better with a steady rate, typically 0.5 to 1% of body weight per week after the first month.
Special considerations: PCOS, thyroid, menopause, and bariatric paths
Insulin resistance looks different across life stages. In PCOS, hyperinsulinemia often drives androgen excess, which worsens ovulatory dysfunction and weight gain. A PCOS weight loss medical program usually blends higher protein intake, targeted carbohydrate timing, resistance training, and medications like metformin or GLP 1 based therapies. Restoring cycles and reducing hirsutism are key markers, not just the scale.
Thyroid dysfunction complicates the picture. Subclinical hypothyroidism can increase LDL and cause fatigue, but it is not the entire reason for weight change in most adults. A thyroid weight loss program doctor will optimize thyroid hormone replacement when indicated, then rebuild habits. Lean mass protection matters even more here.
" width="560" height="315" style="border: none;" allowfullscreen="" >
Menopause and andropause shift body composition. Estrogen decline redistributes fat centrally and can worsen sleep. A comprehensive weight loss clinic will screen for sleep apnea, prioritize strength training, emphasize protein, and consider whether hormone therapy has a place based on risk profile and symptoms. It is not a weight loss drug, but better sleep and mood improve adherence.
For some patients with severe obesity or significant complications, bariatric medical weight loss can serve either as a bridge before surgery or as lifelong care after. Pre bariatric weight loss programs focus on surgical readiness, nutrition education, and shrinkage of liver size for safer operations. Post bariatric weight management prevents weight regain with structured follow up, lab monitoring, vitamin repletion, and, when needed, medication. Even after surgery, insulin resistance can reemerge without support.
What the first three months look like
By the end of the first visit in a modern medical weight loss clinic, you should have a plan, not a pamphlet. We draft a customized weight loss plan doctor approach with four or five anchors: a protein target with meal examples, a carbohydrate range and timing plan, a strength routine with three to five key movements, a cardio prescription that fits into your week, and a sleep goal. If starting medication, we set expectations and titration schedules.
The first month is about stabilization. Hunger steadies. Bloating improves. Some people see a sharp early drop as glycogen and water shift, often 3 to 6 pounds, then a slower slope. By week 4 to 6, most patients with insulin resistance who follow the plan lose 1 to 2 pounds weekly, though percentages are a better gauge. I encourage body measurements and how-clothes-fit checks every two weeks. Body composition scans once a quarter show whether we are protecting muscle.
At 12 weeks, non scale wins stack up: morning energy instead of fog, fewer evening cravings, lower resting heart rate, improved blood pressure, and triglycerides bending down. For those on a GLP 1 weight loss program, we often reach a steadier maintenance dose by the third month, which is when the routine cements.
Plateaus and how we break them
Plateaus arrive even with perfect adherence. The right response depends on the cause. Sometimes steps have slid down without notice. We add a short movement challenge, like 10 minute walks after two meals daily for two weeks, and the logjam breaks. Sometimes protein has drifted low and snacks high. We reset breakfast to 35 grams of protein and anchor dinner the same way. If you are lifting the same weights you did six weeks ago, it is time to progress loads by 2 to 5%. If sleep is poor, cortisol works against you. I would rather trade one cardio session for 30 minutes of earlier bedtime than demand more effort in a sleep deprived body.
When the plan is tight and a plateau persists for more than four weeks, we recheck labs, look for medications that promote weight gain, and adjust the treatment. That might mean modestly lowering carbohydrate range, adding a higher protein day after lifts, or changing medication dose. The key is not to slash calories and hope. We make specific, testable tweaks.
Safety first: medical oversight that earns trust
A clinically supervised weight loss program pays attention to the risks of fast change. On medication, dehydration and electrolyte imbalance can sneak up on you, especially with nausea. We teach patients to prioritize fluids, maintain sodium and potassium through food, and report persistent GI symptoms. Rapid weight loss can increase gallstone risk, so we look out for right upper quadrant pain. In patients with diabetes on insulin or sulfonylureas, we adjust doses to prevent hypoglycemia as food intake and GLP 1 therapy change appetite.
Anyone with a history of an eating disorder needs a careful, team based plan with a therapist. Pregnant or breastfeeding patients require specialized guidance. Older adults need a strong resistance program and higher protein per meal to counter anabolic resistance. Safety is not a paragraph in a consent form. It is a thread woven through every visit.
How to choose a medical weight loss clinic that fits you
There are many options, from boutique practices to hospital based centers. Location matters for access, so people often start by searching for a medical weight loss clinic or medical weight loss near me. Proximity is helpful, but look under the hood. A solid weight management clinic will be transparent, evidence based, and personal.
- Look for a physician supervised weight loss model with board certified clinicians who review your medical history, medications, and labs, not just a coach or a kiosk. Expect a complete initial weight loss consultation with bloodwork, body composition, and a written treatment plan that includes nutrition, activity, sleep, and if needed, medication. Ask how they monitor progress. You want ongoing medical weight loss follow up with access to a weight loss specialist who can adjust dosing, labs at reasonable intervals, and coaching support that adapts, not a one size handout. Clarify medication options. A comprehensive clinic should discuss semaglutide weight loss program, tirzepatide weight loss program, metformin, and alternatives when appropriate, including cost and side effect management. Beware of promises of guaranteed rapid medical weight loss or a fixed weekly number. The best obesity treatment clinic cites ranges, explains trade offs, and tracks health metrics beyond the scale.
A realistic timeline and outcomes you can feel
People ask what to expect. With high adherence to a holistic medical weight loss approach, I often see 5 to 7% body weight reduction by three months, 10 to 15% by six to nine months, and more over a year if medication is used and resistance training protects muscle. Some move faster, some slower. The destination matters less than the slope of the line and the quality of life along the way. Markers like fasting insulin trending down, triglycerides falling by 30 to 60 mg/dL, HDL rising by 5 to 10 points, ALT normalizing if elevated, and A1c shifting out of prediabetes confirm that fat loss is coming from the right places. Waist circumference, not just BMI, tells the tale of visceral fat shrinking.
When we framed Laura’s care as obesity medical treatment, her whole posture changed. In six months, she lost 14% of her starting weight. More importantly, her fasting insulin halved, triglycerides dropped from 210 to 108 mg/dL, and she could carry both grocery bags up the stairs without needing to pause. She learned to front load protein, walk after dinner with her daughter, and lift twice a week. We used semaglutide to quiet the constant hunger, titrated slowly, and dealt with early nausea by pacing meals and increasing fiber. She will tell you the most surprising part was not the number on the scale. It was the quiet in her head around food.
Bringing it together: a simple start while you arrange care
Not everyone can enroll in a comprehensive program tomorrow. While you arrange an initial weight loss consultation, start with a few low risk steps that target insulin signaling and appetite without extremes.
- Eat 30 to 40 grams of protein at breakfast every day for the next two weeks, and include a fruit or vegetable. Walk for 10 to 15 minutes within an hour after two meals daily, even if it is around your living room. Set a 7.5 hour sleep opportunity by turning off screens 30 minutes earlier, and keep a consistent wake time. With each meal, fill half your plate with non starchy vegetables, a quarter with protein, and a quarter with slow carbs like beans or intact grains. Drink water or unsweetened tea between meals, and keep alcohol to one drink on no more than two days per week.
These steps do not replace a doctor supervised diet plan. They do, however, nudge insulin and appetite in the right direction while you secure a place in a clinical weight loss program.
The value of expert guidance, tailored to you
If you have read this far, you already know that a medical diet program is not about perfection. It is about pattern building, course correction, and a team that knows when to push and when to ease off. A comprehensive weight loss clinic should feel like a calm cockpit, not a carnival ride: clear instruments, steady adjustments, thoughtful use of medically assisted weight loss when indicated, and a landing plan that keeps you there.
For some, that includes GLP 1 therapies, a tirzepatide weight loss program, or weight loss injections managed by a weight loss doctor who responds to side effects quickly. For others, it is metformin, a higher protein template, and a renewed relationship with strength training. Often it is a combination at different phases. The goal is long term medical weight loss that holds up when holidays and travel and work stress test your routines.
Insulin resistance does not signal a dead end. It is a pattern your body fell into for reasons that often made sense at the time: stress, sleep debt, certain medications, genetics, a pandemic, shift work. The right medical weight management plan respects that history and writes a new script. Turning the tide is not a single act. It is the cumulative effect of hundreds of small choices, supported by an integrative weight loss program that keeps science in front and shame out of the room.